
Lung cancer screening saves lives
For more information about lung cancer screening at the OSUCCC – James, click or call 1-800-293-5066.
More information Your source for health, wellness, innovation, research and science news from the experts at Ohio State.
Your source for health, wellness, innovation, research and science news from the experts at Ohio State.
There’s a powerful story behind every headline at Ohio State Health & Discovery. As one of the largest academic health centers and health sciences campuses in the nation, we are uniquely positioned with renowned experts covering all aspects of health, wellness, science, research and education. Ohio State Health & Discovery brings this expertise together to deliver today’s most important health news and the deeper story behind the most powerful topics that affect the health of people, animals, society and the world. Like the science and discovery news you find here? You can support more innovations fueling advances across medicine, science, health and wellness by giving today.
Subscribe. The latest from Ohio State Health & Discovery delivered right to your inbox.
Subscribe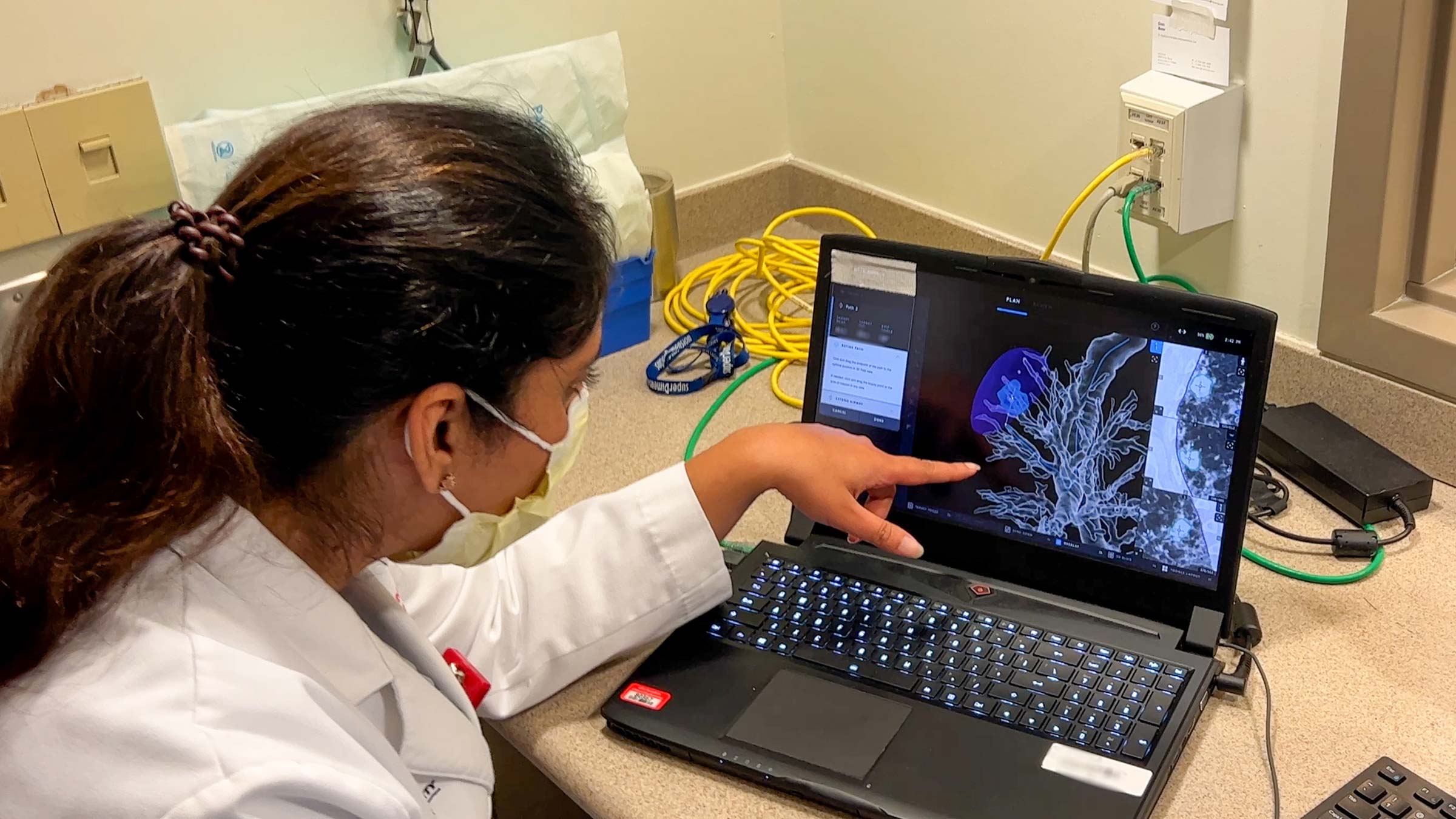
Lung cancer remains the No. 1 cause of cancer-related death in the United States, accounting for almost 25% of all cancer deaths — more than breast, colon and prostate cancers combined.
The U.S. Preventive Services Task Force (USPSTF) recommends annual lung cancer screening for people ages 50-80 who have smoked for at least 20 years, but only 5.7% of eligible Americans were screened for lung cancer before the COVID-19 pandemic.
“For people who are at increased risk for lung cancer due to smoking history, waiting until they experience symptoms — like trouble breathing, a chronic cough or chest pain — will be too late. This is why lung cancer is so deadly. These are often signs that the disease is impacting the airways and has advanced to stage 4, which has fewer treatment options,” says Michael Wert, MD, a pulmonologist and director of the lung cancer screening program at The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (OSUCCC – James). Dr. Wert is also a clinical assistant professor of internal medicine at the Ohio State College of Medicine.
“Lung cancer screening is a critical tool for detecting these cancers in their earliest stages, when they are treatable. I implore anyone who is at increased risk to ask their doctor about this simple screening tool.”

Steve Porter had recently quit after nearly 50 years of smoking cigarettes. When his doctor suggested starting annual lung cancer screening as a precaution due to his history of smoking, noting that his insurance would cover the test, he didn’t hesitate — “Sure, sounds good.” That was in 2017.
In 2019, the screening test showed a nodule that could be a sign of early cancer, which was monitored closely. Three years later, the nodule had changed enough to warrant a biopsy that confirmed stage I lung cancer.
“I feel grateful my doctor recommended that lung cancer screening, because it wasn’t something I realized was available to me,” Porter says. “I was always told the earlier you find it, the better your odds of beating it. And it proves that fact here, because it was a slow-growing cancer, and I'm cancer free now, for right now, so that's a good thing.”
He encourages anyone with a significant history of smoking to get screened — and do it now.
“So many people put off screening because they aren’t feeling bad — but if you put it off until you feel sick, it is going to be too late with lung cancer. If you are at high risk because of smoking history, you need to face it. It could save your life,” he says.
Lung cancer screening is now covered by many insurance plans for individuals who are deemed at higher risk, per USPSTF screening guidelines.
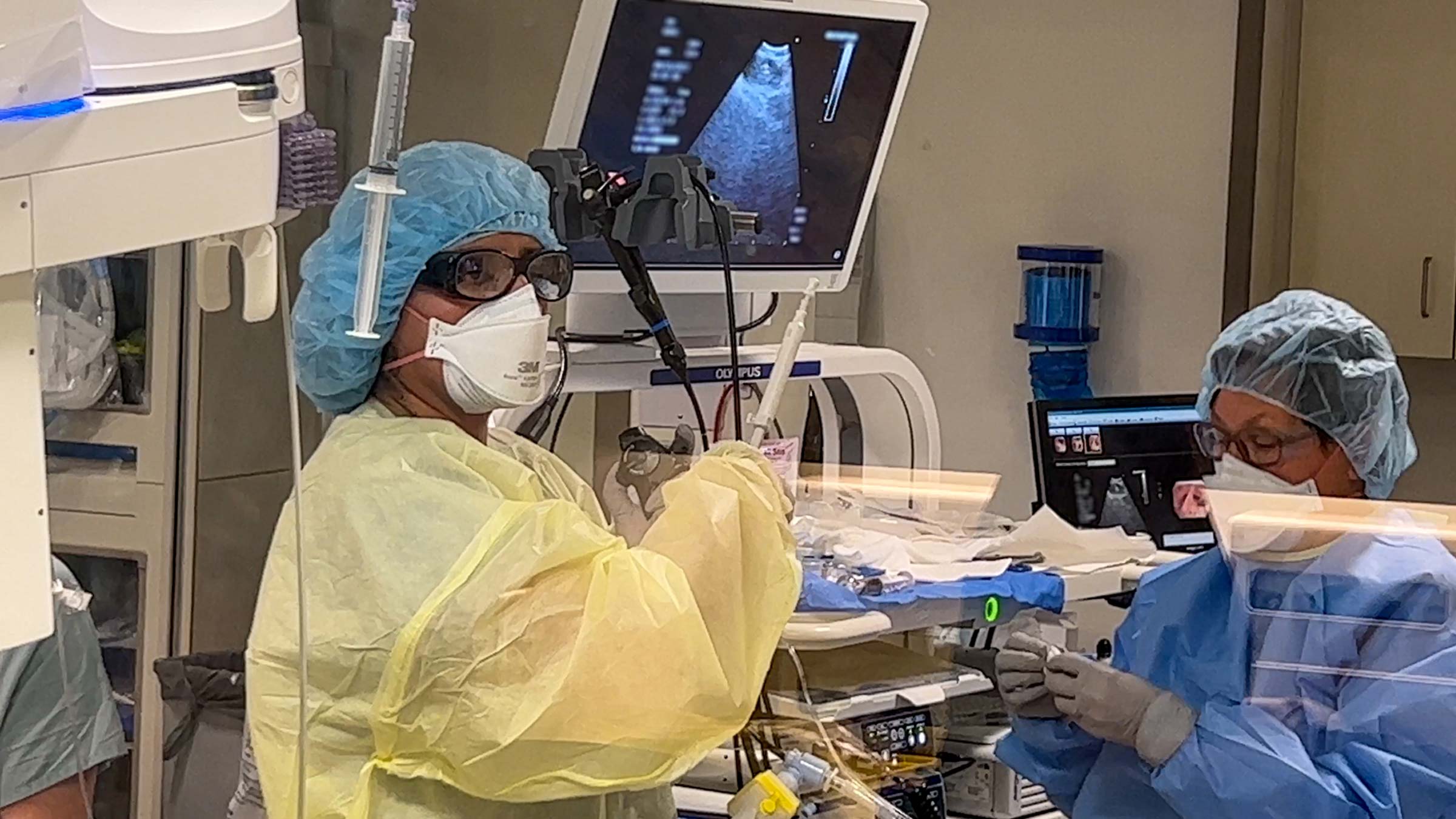
Screening the highest-risk individuals provides the best chances of identifying lung cancer in its earliest stages, but an imaging test commonly used for detecting injuries and illnesses can also catch the subtle, early signs of lung cancer, say experts at the OSUCCC – James.
While computed tomography (CT) scans can provide important information to diagnose other illnesses and conditions, these imaging tests can also reveal other unrelated issues, known as “incidental” findings, that raise questions beyond what the physicians were originally looking for.
Launched this year as a collaboration of the OSUCCC – James and The Ohio State University Wexner Medical Center, the Lung Nodule Program was established to create a system for capturing incidental chest CT lung nodule findings — with the aid of machine learning tools — to determine which patients need additional evaluation.
Jasleen Pannu, MBBS, clinical assistant professor of internal medicine at The Ohio State College of Medicine, who leads this new effort, estimates that roughly 10% of all lung nodules identified through chest CT scans performed to investigate other conditions are cancerous; however, determining which spots need additional evaluation can be challenging. At a large health system like Ohio State, that could mean 1,000 early-stage lung cancer diagnoses annually.
“We do not want any of these cases to be missed, so creating a process to pinpoint precisely who may benefit most from a biopsy is critical,” Dr. Pannu says. “It is a balancing act of providing the appropriate level of follow-up testing for each patient while also working within the significant staffing resources needed to gather, assess and triage a large volume of incidental findings in a timely way.”
Lung cancer screening remains the best defense for those at higher risk for lung cancer. In 2021, the USPSTF updated its lung cancer screening recommendations to include annual screening for lung cancer with low-dose CT scans in adults between the ages of 50 to 80 years who have a 20 pack-year smoking history and currently smoke or have quit within the past 15 years. Lung cancer screening is now covered by most insurance plans, but it’s best to check with your provider.

For more information about lung cancer screening at the OSUCCC – James, click or call 1-800-293-5066.
More information