Game-changing tools train emergency medicine students and residents to respond to real-life disasters

The Ohio State University College of Medicine is using virtual reality (VR) and high-tech manikin simulators to help prepare learners for real-world, emergency situations. “From drawing blood to defibrillation to codes, simulation allows learners to practice procedures and make quick decisions without life-and-death consequences,” says Jay Read, associate director of Ohio State’s Clinical Skills Education and Assessment Center (CSEAC).
While most simulations take place in the 3,000 square-foot leading-edge center on campus, sometimes, a real-world setting is required.
Two recent training sessions — one simulating a virtual subway station bombing, the second simulating an airport disaster — gave medical residents and students the opportunity to work through the fast and chaotic nature of a disaster to fine-tune their responses and decision-making.

Students go to the ‘virtual underground’ for subway bombing simulation
In March, students studying emergency medicine donned VR headsets to enter a virtual subway station moments after a bombing as part of their disaster response training. The session was held in the EdTech Virtual Reality Zone in the Prior Health Sciences Library. In addition to being easily accessible, the virtual program is more cost-effective than disaster drills that rely on mock patients and manikin simulators.
As part of a simulated Emergency Medical Services (EMS) team, students triaged patients, evaluated injuries and provided medical treatment in the all-virtual environment. Afterward, they were evaluated on their ability to sort patients and accurately access and treat their injuries.
The accessible, virtual program was designed by Douglas Danforth, MD, associate professor of Obstetrics and Gynecology at the College of Medicine, who works with virtual reality, and Nicholas Kman, MD, an emergency medicine physician at The Ohio State University Wexner Medical Center. This training is supported by a grant from the Agency for Healthcare Research and Quality.
Creating a ‘flight plan’ for addressing airport disasters
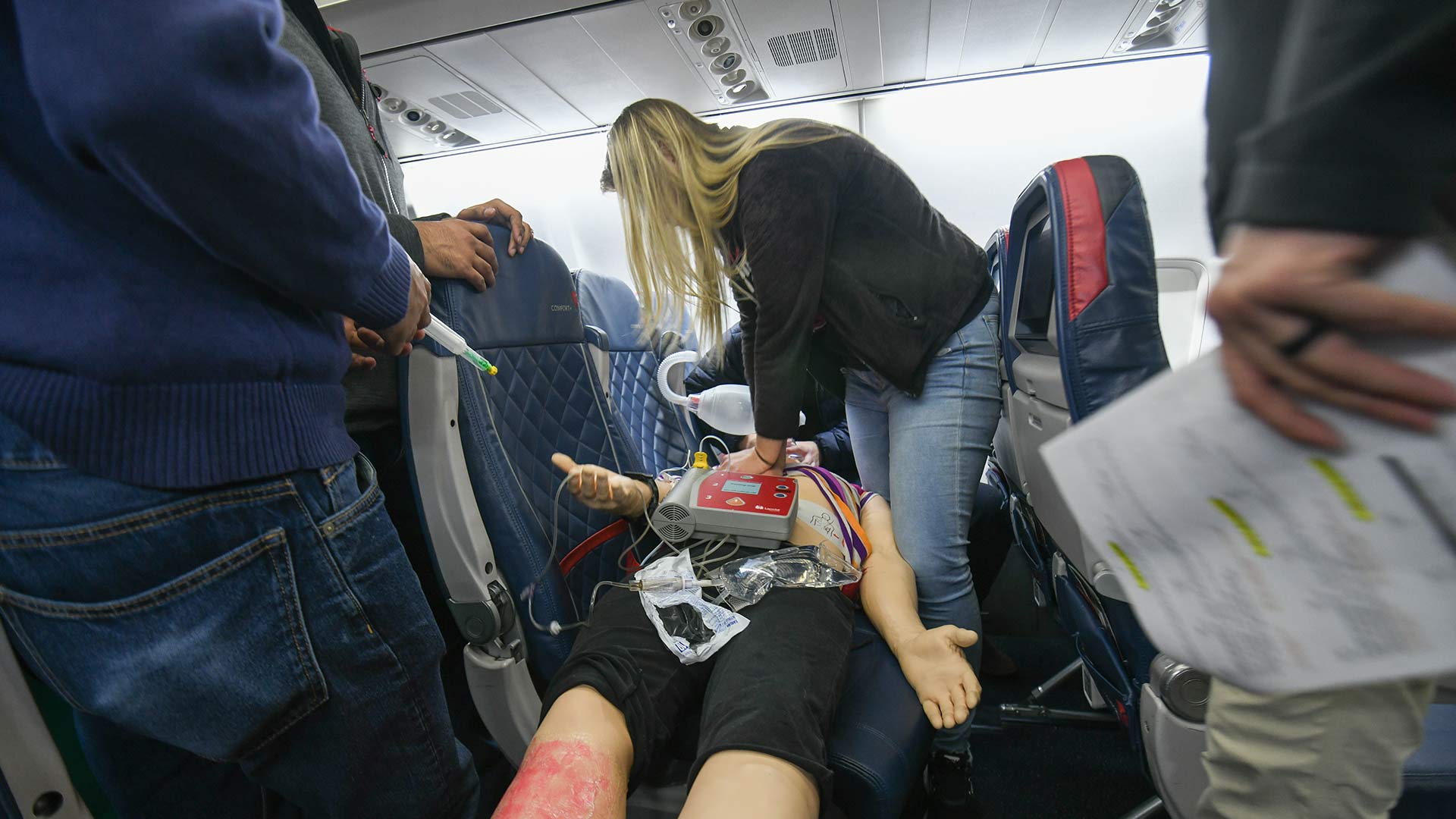
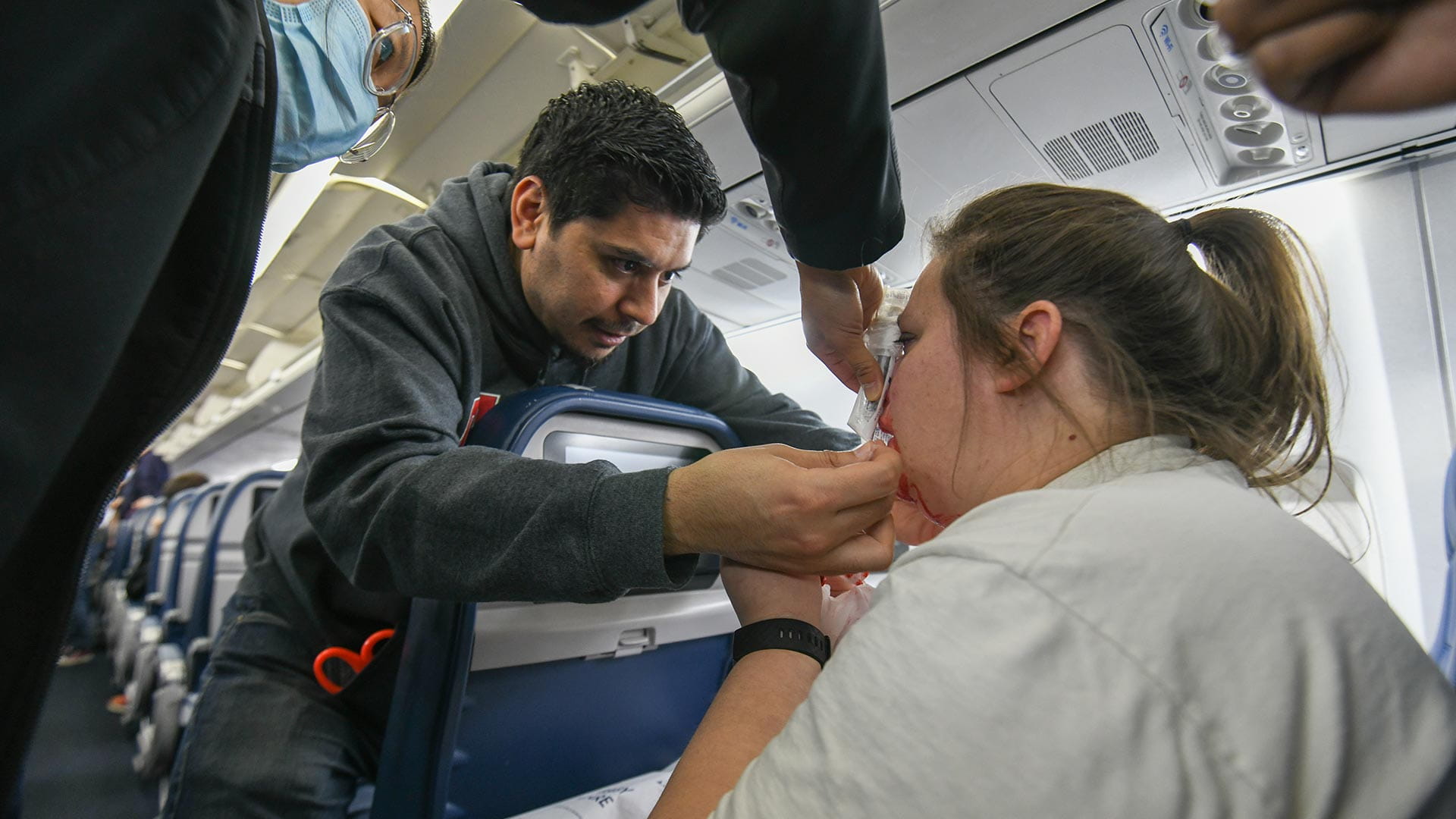
In April, emergency medicine residents spent an overnight cycling through eight different emergency scenarios on an airplane and a jetway gate at the John Glenn Columbus International Airport. Emergency room physicians, members of the CSEAC, including Shery Pfeil, MD, medical director of the CSEAC and professor of Internal Medicine at the College of Medicine, joined simulationists to put emergency medical residents through emergency scenarios and drills with human and high-tech manikin subjects.
They practiced treating passengers in cramped spaces with limited supplies for conditions such as severe allergic reaction, loss of consciousness, cardiac arrest, nosebleeds, mental health crises and more.
Simulationists used software to change vitals, such as pulse and breathing, on the manikins to teach learners how to react and adjust care protocols. Through a debrief after each scenario, learners were able to ask questions and receive feedback on the choices they made or could have made during the drill.

The future of medicine is at Ohio State
Our innovative curriculum, life-altering biomedical research and unsurpassed patient care make us one of the top medical schools in the country.
Explore our programs