Helping wounded veterans experience life with less nerve pain
Military Medicine Program offers multiple ways to treat nerve damage, a common and complicated problem
Over 100 feet from the ground, Shane Jernigan knew his parachute wasn’t going to open.
Something had gotten stuck within it. Instead of drifting to the ground, he knew he’d slap it. All the way down, he screamed an expletive, his mouth wide open.
He hit the ground, feet first, then backside, then legs and still holding the rifle that had just rammed and broken his shoulder.
“I assumed I was dead,” he says.
Around him, he could see other members of his troop, some still floating down in their parachutes, some already landed.
OK. I’m not dead.
He fell back on the grassy ground.

It was the summer of 1994. Jernigan was near Jacksonville, Florida, at a U.S. Army base rehearsing the invasion of Haiti that was to come. He was 22.
That would be the first of three accidents during Jernigan’s early years in the military. He would recover from all three and go on to become an elite athlete, but the lingering effects of his injuries and chronic pain would prove to be unbearable.
Fortunately for Jernigan, he discovered the Military Medicine Program at The Ohio State University Wexner Medical Center and the unique talents of surgeon and fellow veteran Jason Souza, MD.
Nerve damage leads to lasting trauma
Jernigan was a U.S. Army Ranger, a member of a force that carries out Special Operations raids and assault missions on enemy grounds. They’re the toughest of the tough in the Army where Jernigan learned: Even if you’re in excruciating pain, even if you’re unsure you’re going to make it, don’t scream, don’t cry, don’t lose your composure. Stay focused on the mission.
So, after hitting the ground that summer day in 1994, he got up, ignoring the bleeding from his mouth and what he was sure were broken bones in his legs. He rolled up his parachute and began walking.
The stoicism Jernigan learned in the Army stayed with him through surgery after surgery, and through all his efforts to rehabilitate his back and limbs by competing first in marathons, then ultramarathons, then triathlons.
The more he biked, the better his knees felt. The more he ran, the better his spine felt. And the prospect of not doing well in a competition motivated him — even if he felt like he couldn’t stand up — to get out of bed and train. Sports helped, but only to a point.
“I would go out and hike, sometimes mountain climb, and at the end of the day, it felt like I was being shot in the leg with a police taser — repeatedly,” says Jernigan, 51.

That leg, his left one, was amputated four years ago. Over time, the injuries to his leg — which started with the parachute ordeal and continued with accidents that re-injured his ankle and knee — left him unable to walk.
But long after Jernigan’s leg was amputated, pain still shot through it, especially at the end of every day. Most nights, he slept for 15 to 20 minutes at a time before waking up again in pain.
Last spring, decades after the parachute accident, Jernigan drove from his farm in Grand Rapids, Ohio, southwest of Toledo, to the Ohio State Wexner Medical Center.
He met with Dr. Souza, a plastic surgeon who specializes in restoring and reconstructing injured limbs and resolving problems after limbs are amputated. Dr. Souza is central to Ohio State’s Military Medicine Program, which offers a multidisciplinary team of surgeons, physicians and other providers experienced in caring for service-related trauma.
A veteran of the Navy, Dr. Souza spent six years caring for wounded warriors at Walter Reed National Military Medical Center before coming to the Ohio State Wexner Medical Center. He understands the complexity of treating both the visible limb injury and the invisible nerve pain that often comes with it.
“The challenge constantly pushes me to be better and more innovative as a surgeon,” Dr. Souza says. “Conventional surgical strategies too often fail to get my patients the outcomes they’re counting on.”
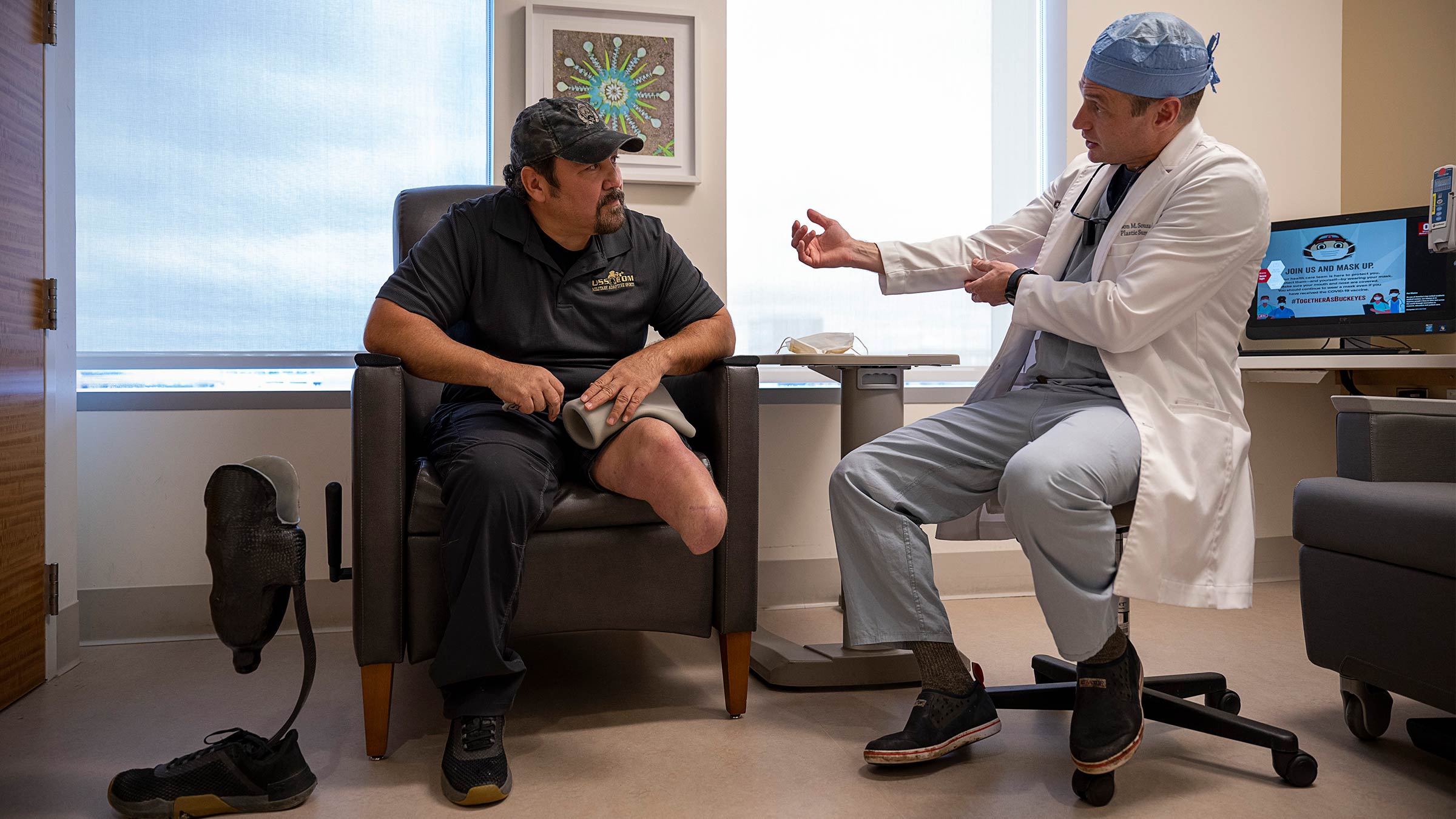
Operation resolves chronic pain
Last year, Dr. Souza operated on Jernigan’s left leg to reduce his pain by reshaping the remaining limb to better fit into his prosthesis. He rerouted Jernigan’s injured nerves through a procedure known as targeted muscle reinnervation (TMR). TMR aims to eliminate or significantly reduce pain after an amputation by reconnecting broken nerves. As part of the TMR procedure, the nerves that used to go to the top and bottom of Jernigan’s foot were rewired to connect to muscles remaining in his calf, above the amputation. Weeks after surgery, the burning pain Jernigan had started experiencing when his leg was amputated no longer bothered him.
Dr. Souza and the Ohio State Wexner Medical Center have been at the forefront of advances in managing pain after an amputation.
“There’s no greater reward for a reconstructive surgeon than to see a salvaged limb or optimized amputation put to good use,” Dr. Souza says.

Why pain doesn’t always end with amputation
Nerves are like wires. They carry electrical impulses from the brain and spinal cord to arms, legs and other parts of the body to allow you to move a body part and feel sensation. But nerves don’t recognize when a limb is amputated. The nerves will try to continue to send electrical impulses to parts of the body even after they’ve been amputated.
If nerves are injured or cut, such as during an amputation, it’s like cutting an electrical wire — the electrical impulses are still there but have nowhere to go. When the nerves that typically carry signals throughout the leg are blocked from trying to send signals to the lower portion of the leg, which was amputated, they can sometimes form a tight ball of disorganized nerves at the edge of the amputation. That’s called a neuroma. It causes extreme and often debilitating pain called phantom limb pain.
About 65% of people who have amputations experience phantom limb pain, which feels like it’s coming from the body part that’s no longer there, Souza says.
This pain is not well understood. It’s believed to be caused by pain signals from the damaged nerves that had activated the portion of the body that was amputated. Another source of that pain is the absence of healthy feedback between the brain and the nerves from the part of the body that was amputated.
Restoring the body’s electrical circuit
In the past, efforts to treat phantom limb pain focused on cutting, crushing, burning or burying the nerves severed in the amputation. However, these techniques seldom prevent the nerves from sending problematic pain signals to the brain. They also don’t restore healthy feedback between the nerves and the brain.
In a TMR surgery, the nerves cut during an amputation are reattached to small nerves within muscles in the remaining portion of the limb. As a result, those previously broken nerves that once controlled the muscles of the amputated part of the leg can direct their signals to muscles in the portion of the leg that remains. That stops or significantly reduces pain signals previously sent out by broken nerves.
With reduced pain, patients potentially need less pain medication over time, and they may be able to wear a prosthetic limb more effectively.
Jernigan has found that to be true.
Two weeks after surgery at Ohio State, his left leg no longer felt like he was being shot with a taser, but instead like the pain of hitting his funny bone over and over — constant but minor.
Six weeks after surgery, wearing a prosthetic leg, he completed a triathlon.
Six months after surgery, he hardly noticed any pain.
“It’s leveled out so much,” he says. “It’s more like a tingling now.”

Chronic nerve pain, a hidden problem
Constant nerve pain is not only a problem for someone who has lost a limb. Any soldier who suffers an injury to a leg, arm or another body part has also likely suffered damage to the nerves. Sometimes this leads to numbness or keeps someone from being able to use or fully use a limb or appendage. Often, nerve damage leads to excruciating pain.
However, that nerve damage doesn’t show up on an X-ray. So, despite the intense pain the frayed nerves may cause, the source of the pain often goes undetected and insufficiently treated.
“Patients and doctors often focus on the wounds, and they focus on the fractures, because you can see them,” Dr. Souza says. “What’s much harder to identify and understand is the nerve injury that comes with those wounds and fractures.”
Injuries to sensory nerves are especially likely to be overlooked, he says. These nerves send signals to the brain to allow you to feel, taste, smell and see. When they’re injured, a body part may go numb, or experience a tingling feeling or pain.
“It’s a pain that makes people want to cut off their limbs,” Dr. Souza says.
Injury to a motor nerve, a nerve responsible for moving body parts, is typically easier to diagnose than a sensory nerve injury. Someone with a motor nerve injury usually will report not being able to move the injured limb. With injury to a sensory nerve, the person often can still move that body part.
Without an MRI, ultrasound or dedicated nerve study, a doctor can only diagnose nerve pain through a physical examination.
“I see a common pattern with nerve pain. When I touch a sensitive spot, the patient’s eyes get wide and the patient jumps,” Dr. Souza says. “There are few other pains that trigger this involuntary reflex.”
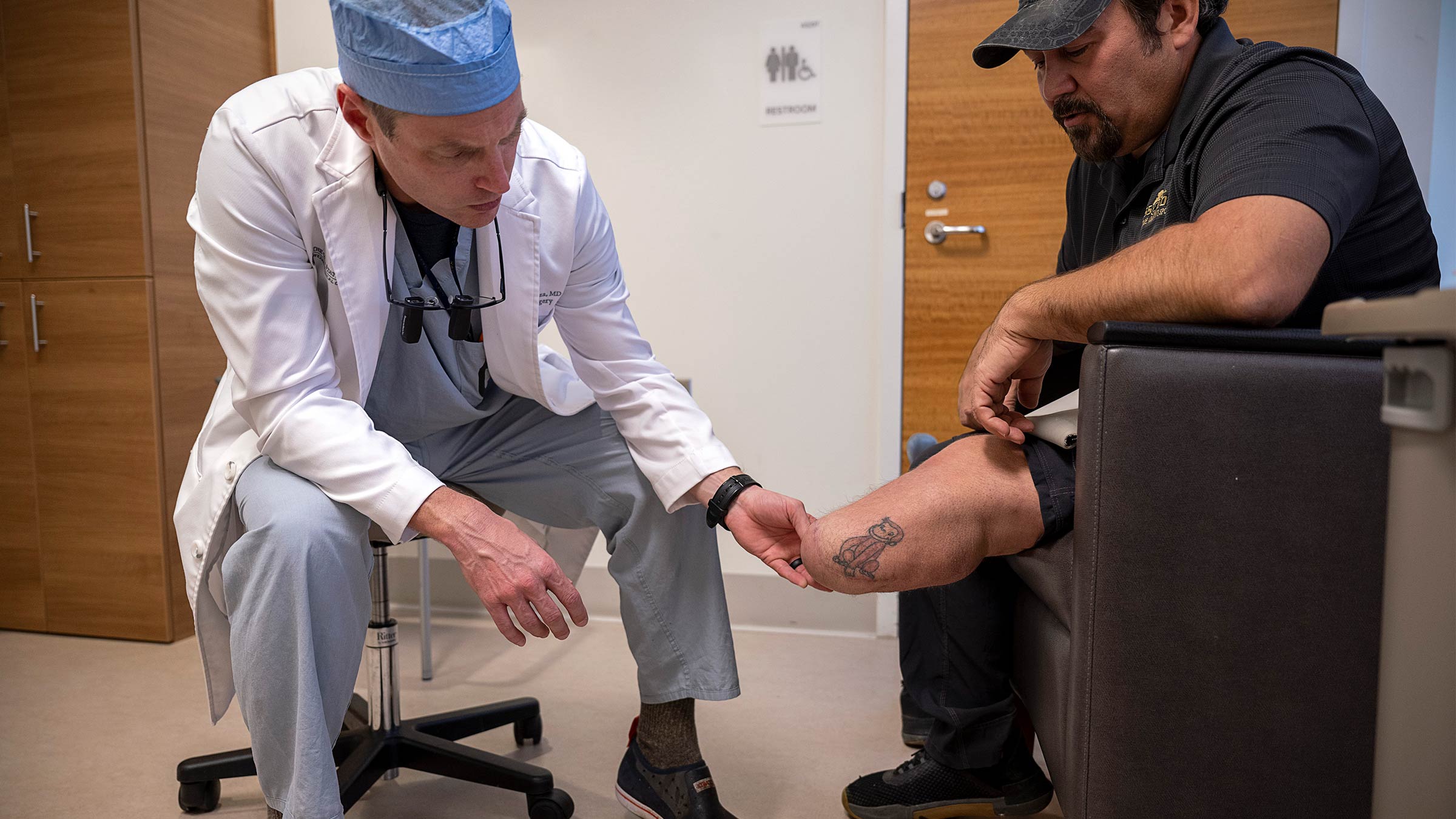
A team approach to treating nerve pain
Relatively few physicians specialize in managing nerve pain. Treating it can be complicated, which is why the Ohio State Wexner Medical Center offers a range of treatments: surgeries that reconstruct and rewire nerves, physical therapy to retrain the nerves, behavioral therapy and mental health strategies.
Other interventions include spinal cord stimulation, in which a device implanted within a person’s abdomen or buttocks sends low levels of electricity into the spinal cord to block pain, and another method called pump placement, which sends medication directly to the spinal cord via a small pump inserted under the skin of the abdomen.
“It’s not unusual for people to go for years being told there's nothing you can do, because their pain is hard to understand and even harder to treat,” Dr. Souza says.
“We certainly don’t have all the solutions, but we have found that a team approach and a willingness to explore new strategies have been key to many of our patients improving.”
It no longer takes Jernigan two hours to get his prosthetic leg on or off because of pain. At night, he’s stopped waking up screaming from a recurring nightmare of the parachute accident and slamming, all over again, onto the hard ground.
He attributes the ketamine he received during the surgery and immediately afterward with improving his sleep and mental health overall. Ketamine is an anesthetic that triggers hallucinations while it reduces pain. The drug is being used during some nerve surgeries because of its pain relief and mental health benefits, Dr. Souza says.
“It’s part of our efforts to treat not only the broken nerves, but also the brain’s processing of pain signals from those injured nerves,” he says.

The healing power of the mind
Four years ago, Jernigan began competing on a military team of para-triathletes. They’re all determined, like Jernigan is, to always have a goal, or several, in front of them.

Sometime in the next couple of years, Jernigan aspires to return to college. He wants to study the power of the mind to overcome pain, both physical and emotional.
Though retired from the military, he still trains soldiers to prepare them for special missions. Recently in New Mexico, he was riding in a helicopter with several other Army Rangers and getting ready to jump out along with them. This time it was not far, just 3 or 4 feet from the ground.
As they were given the 1-minute warning, Jernigan realized he had never jumped out of a helicopter with a prosthetic leg.
How can I jump with only one leg?
Three, two, one.
He stepped out into the hot, dry air. Muscle memory took over. His legs knew just how to land. Then he got up, surprised that it all went OK, and continued with the mission.

Unparalleled care for wounded service members
Explore Ohio State’s Military Medicine Program
Learn more



