After decades without options, new hope for swallowing disorders
Experts in dysphagia, known as swallowing disorders, are pioneering treatments and research to restore the joy of eating.
It must have been a fluke, Randall Wright figured.
He was with his wife and friends at a hibachi restaurant when he coughed, and the rice and veggies he’d been eating came out his nose.
“I don’t get embarrassed easily,” he says. “But I didn’t want to make other people uncomfortable. I didn’t eat anything else after that.”
Then it kept happening, about once a week, enough that whenever Wright ate, he was on guard with napkins, ready to wipe his nose. Food sometimes stuck at the back of his mouth.
“I could still taste what I had for breakfast eight hours earlier,” says Wright, 63, an IT manager who lives in Charleston, West Virginia.
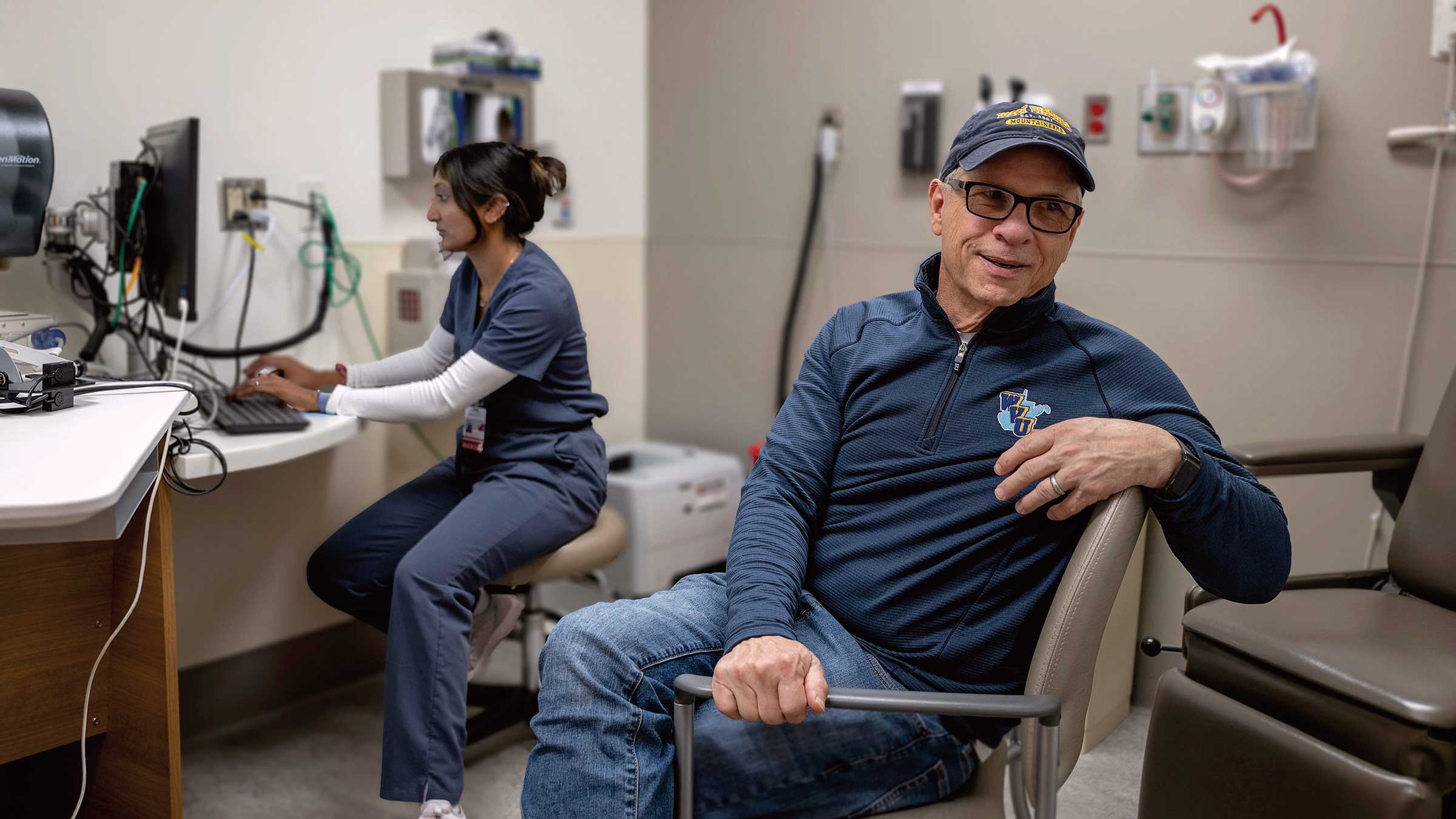
Restoring the joy of eating after a swallowing disorder
Wright began having trouble eating after he received radiation for neck cancer in late 2018 and early 2019. Radiation saved his life, but it also harmed some glands that make saliva, leaving his mouth dry. It damaged some of the nerves and muscles he needed to swallow, too. The small valve that should keep food out of his nose stopped closing all the way.
Wright hoped his swallowing problem, also known as dysphagia, would go away – or that he could learn to live with it.
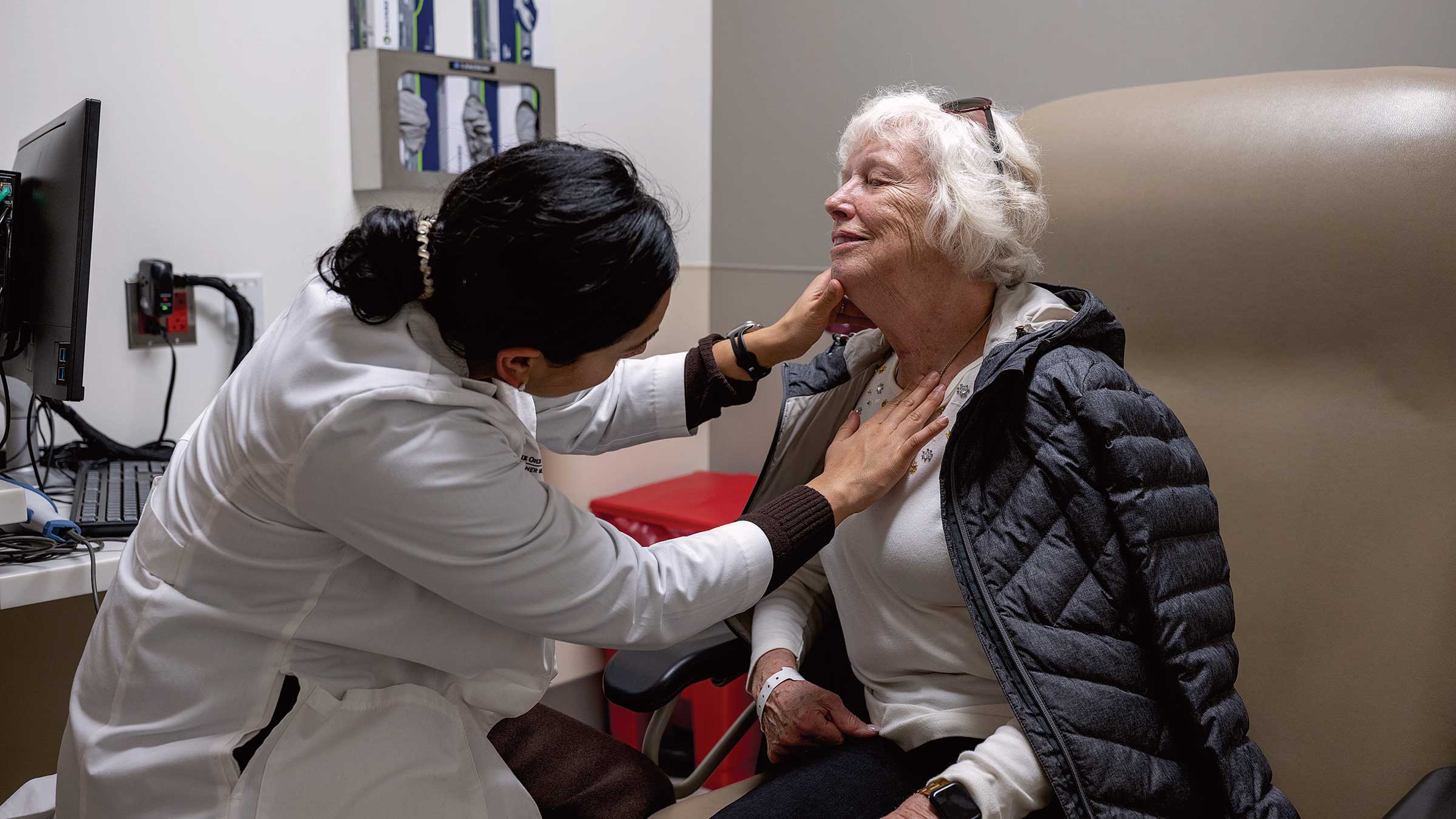
“Eating is this unconscious, enjoyable process. But for many of my patients before treatment, eating is a very stressful process,” says Apoorva Ramaswamy, MD, a throat surgeon and dysphagia specialist at the OSUCCC – James.
“They’re worried about things going down the wrong way, things getting stuck, having to cough, making the people around them feel awkward. The biggest goal is to make eating an easy, enjoyable process again. And we’re able to do that,” says Dr. Ramaswamy, who’s also a clinical assistant professor in the Department of Otolaryngology – Head and Neck Surgery at The Ohio State University College of Medicine.
Dr. Ramaswamy leads a team of speech and language pathologists, dietitians, physical therapists and social workers.
“There’s a lot we can treat, and it makes a big difference for many people. The tools at our disposal have greatly evolved,” Dr. Ramaswamy says.
Uncontrolled swallowing can turn meals into medical risks
Swallowing is a common problem for people who have had radiation to eliminate cancer anywhere on their head or neck. On average, 70% of people with head or neck cancer will have trouble swallowing at some point, sometimes a year or two after their radiation ends.
Even people who’ve never had cancer can develop dysphagia. Brain disorders such as MS, ALS, stroke or dementia can cause swallowing problems. So can untreated acid reflux.
While dysphagia is most common in seniors, more middle-aged and young adults are now being diagnosed with the disorder. The rise is linked to increases in human papillomavirus (HPV)-related cancers in the head and neck, and also to an allergic disorder that inflames the esophagus.
Dysphagia can not only make it difficult for people to eat or drink – it can be life-threatening.
Nearly one-third of people with head and neck cancer develop aspiration pneumonia, an infection caused by food or water going into their lungs. About 30% of those who develop it die within the first year. And yet, for decades, few options were available to resolve or even improve swallowing problems.

Team approach offers hope to patients with dysphagia
In 2021, the Ohio State Wexner Medical Center opened the first-of-its-kind clinic treating patients with head and neck cancer who develop difficulty swallowing. The focus has since widened, so people can be treated for a swallowing problem arising from any type of disorder.
Through the clinic’s efforts, more people can now swallow and speak better as a result of exercises, medication, surgery or other procedures.
“At least once a week, I’ll have tears come to my eyes because a patient who’d been on a feeding tube will tell me they ate food through their mouth for the first time in several years,” Dr. Ramaswamy says.

How voice and swallowing connect
Wright repeats a series of sounds as speech pathologist Tulsi Vira records him:
Papapa, Kakaka, Tatata, Sasasa.
How clearly Wright can say the sounds also indicates how well he’s able to swallow. The same muscles in the soft palate at the back of his mouth that are supposed to keep food and liquid out of his nose when he swallows also can affect how he talks. If the soft palate isn’t working properly, too much sound will escape his nose instead of his mouth, causing nasal-sounding speech and often trouble swallowing.
Keykeykey, Ccc, Shesheshe, Mamama, Nanana.
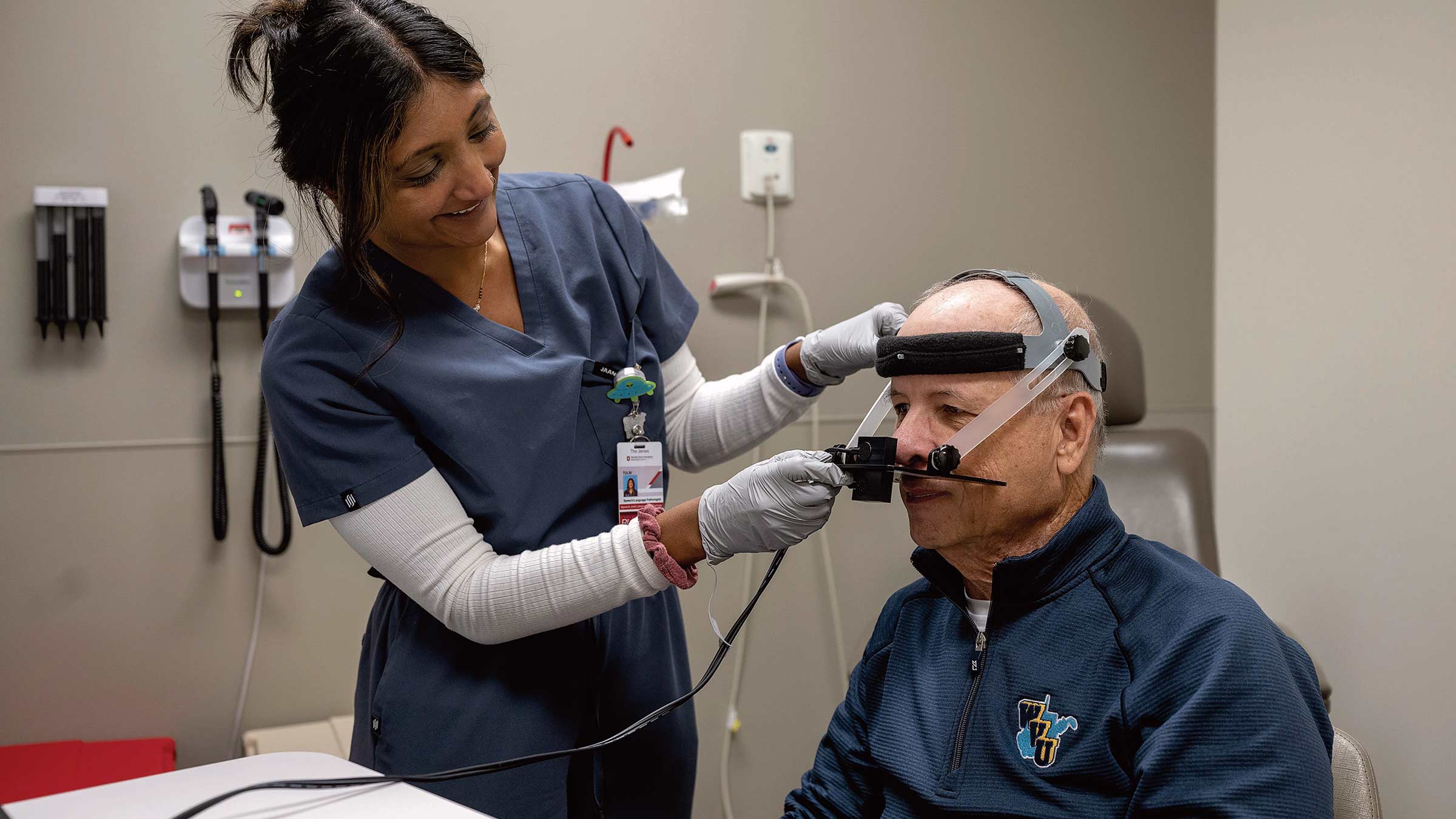
In October 2025, Dr. Ramaswamy widened Wright’s esophagus and closed the passage between his nose and mouth to help block food from going from his throat to his nose. It was the second surgery she did to resolve a common problem among people treated for head or neck cancer.
Wright may need to have the procedure done again in a few years because scar tissue from radiation can continue to tighten and narrow the passageway over time.
Ah, Eeee, Ssss, Mmmm.
The test results show his voice is pretty much the same before and after the surgery, meaning Wright might benefit from regular speech therapy to strengthen his swallow muscles. Still, he’s better able to keep food from going into his nose, which is Wright’s main concern.
Preventing swallowing problems
A key leader on the dysphagia treatment team at Ohio State also works to prevent the disorder. Emily Plowman, PhD, CCC-SLP, a speech-language pathologist and world-renowned dysphagia expert, assesses people before open heart and lung transplant surgeries to determine the likelihood of them developing dysphagia as a complication from general anesthesia and surgery.

Dr. Plowman’s research on a cardiac intensive care unit led her to develop an algorithm model that allows medical providers to predict a person’s risk for developing dysphagia after surgery.
A breathing tube used during surgery can irritate or injure the parts of the throat that help you swallow. Also, during heart surgery, a nerve that wraps around the heart’s main artery and helps you speak and swallow can be damaged, leading to dysphagia.
As a result, some people experience silent aspiration following surgery. Food or liquids go into their windpipe without triggering them to cough it out. They may not even be aware of it happening.
“We call it the silent threat to recovery,” says Dr. Plowman, who’s also a professor of Otolaryngology – Head and Neck Surgery at the Ohio State College of Medicine, and director of the Aerodigestive Research Core laboratory.
When a patient breathes food, liquid, or saliva into their lungs without coughing it out, they can suffer serious health problems, including pneumonia.
“If we can determine who’s at highest risk of a swallowing problem after surgery, we can pay close attention to them,” Dr. Plowman says.
Along with predicting dysphagia risk and taking steps to prevent it, Dr. Plowman and her colleagues are testing a novel screening tool for nurses to use with someone recovering in the intensive care unit after surgery, to detect if they’ve developed dysphagia.
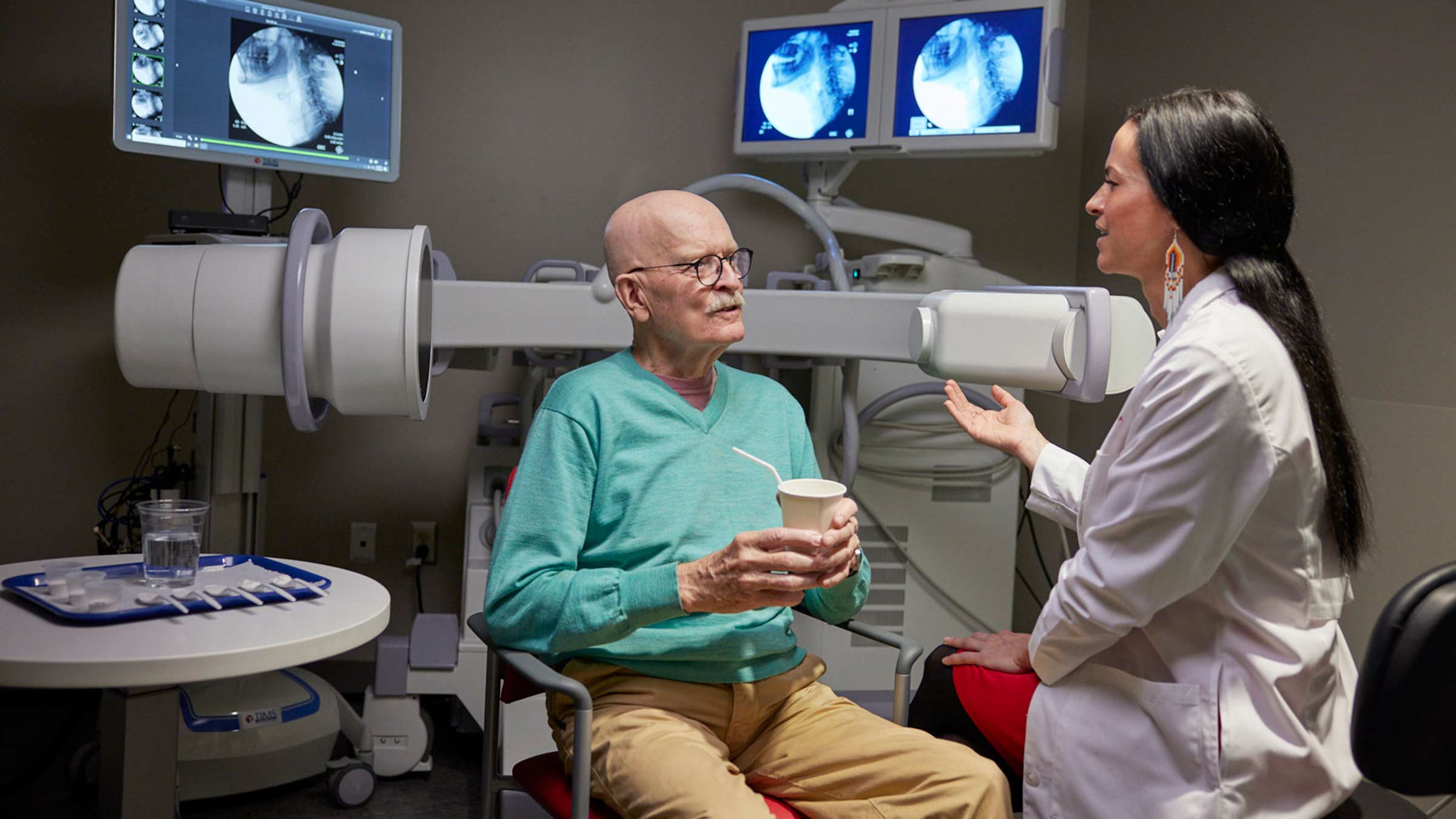
Pioneering new treatments for dysphagia
Swallowing trouble can vary from food and liquids slipping out the lips or nose to not having enough saliva, causing food to get stuck in the throat. As a result, Ohio State’s dysphagia clinic offers a wide array of treatment options ranging from guided exercises to injections to surgical procedures.
People who have trouble swallowing often need ongoing treatment. It’s not always possible to completely restore someone’s ability to swallow. But significant improvements can often be made so someone no longer requires a feeding tube, needs it less frequently or can finally eat solid foods after months of having only liquids.
“Being able to eat meals again can make a huge difference in someone’s life,” Dr. Plowman says.
It has for Wright. Every couple of years, he'll need to have some type of procedure to help him swallow better, but he's OK with that. He's just glad the treatments work.
“Eating is a lot easier,” he says. “It used to be every time I took a bite of food, I’d cough.”





