
In 2019, everything changed for Philip Knisely. Nearly a decade earlier, he’d been diagnosed with liposarcoma, a rare type of soft-tissue cancer that starts in fat cells. It typically causes masses to develop as lumps under the skin, and they require surgery or sometimes radiation treatment.
Knisely had undergone numerous surgeries over the years to remove recurring, painless tumors that would appear in or near his groin. Those procedures were “annoying, but fairly straightforward,” he says.
After each surgery, he’d rest for about three weeks and move on. He continued his normal life, dutifully walking 10,000 steps a day, spending vacations in Provence — strolling France’s small-town, cobblestone streets — and chasing his five grandchildren on the beach of Hilton Head Island, where he and his wife lived part of the year.
But in 2019, he knew things were different. He began to experience constant pain that spread through his hip and groin, making it difficult to walk, sleep and work. By spring 2020, Knisely had already lost significant amounts of muscle tone in his right leg, eventually dragging it as he walked.
The stakes became obvious. The cancer needed to be removed, but with a tumor that came into contact with his femoral nerve, he needed a surgical team that could renew his hopes of more beach games with his grandchildren and walks in the south of France.
“It was clear that the next surgery was going to be much more involved,” Knisely says.
“And because of this tumor’s location, we knew that my mobility would likely be affected afterward. This surgery was potentially going to be a change in my quality of life, which had already diminished significantly.”
So Philip Knisely began his search.
A life-changing choice
His home base was Chicago, but Knisely’s 10+ surgeries to remove tumors had taken place at multiple cancer centers throughout the United States. A consummate comparison shopper, he collected reviews and research, then interviewed care teams before making decisions about procedures that could have lifelong effects.
It’s how several of his surgeries landed in the hands of Raphael Pollock, MD, PhD, who performed the initial procedures at a different institution but now serves as director of The Ohio State University Comprehensive Cancer Center – James Cancer Hospital and Solove Research Institute (OSUCCC – James).
“Following Dr. Pollock was an easy decision,” Knisely says. “I’d gotten great care, and he’s incredibly knowledgeable and one of the most empathetic surgeons you’ll ever meet. But I spent a lot of time getting to know his team at Ohio State and interviewing teams at other health centers, too.”
One institution, Knisely says, wanted to use radiation therapy first. At Ohio State, the team was focused on saving a radiation option for later.
“I interviewed every single member of the team — Dr. Valerie Grignol, Dr. Roman and Dr. Amy Moore the most,” he says. “The Ohio State team was much younger than other teams I talked to, but they were so prepared and confident that they could not only relieve me of pain and of cancer, but also restore some of my quality of life.”
The collaborative difference of Ohio State
Ohio State provides a multidisciplinary approach that includes top-notch cancer surgeons and plastic and reconstructive surgeons. Together, the surgical teams plan the tumor resection to not only safely remove the tumor, but also to preserve structures, including nearby nerves, to prepare for nerve transfers that can restore function to patients’ limbs.
Valerie Grignol, MD, is a surgical oncologist at the OSUCCC – James who specializes in sarcoma, including the liposarcoma Knisely was diagnosed with. She credits her ability to more effectively serve patients like Knisely to Amy Moore, MD, chair of The Ohio State University’s Department of Plastic and Reconstructive Surgery.
A surgeon who’s world-renowned for her skill in peripheral nerve surgery, nerve repair and nerve regeneration, Moore had just joined Ohio State in November 2019.
“Working with Dr. Moore has allowed us to offer operations that weren’t available to patients before,” Grignol says.
“Her ability to reconstruct nerves is particularly important for sarcoma patients, where nerve involvement can really be prohibitive to performing a surgical resection, when we know that the complications could negatively impact their quality of life — to the degree that resecting the tumor doesn’t make sense for a patient.”
In Knisely’s case, this collaboration meant everything.
In his first meetings with Grignol and with Roman Skoracki, MD, an oncologic plastic surgeon at the OSUCCC – James, the two surgeons were candid about potentially being unable to remove the cancer cleanly from the body without also removing some portion of the nerve. The tumor had clearly infiltrated the femoral nerve that allows for leg function.
“They said they wanted to bring Dr. Moore in to be there for me in the OR, and these collaborative decisions made all the difference,” Knisely says.
The team collaborated not only with one another, but also with Knisely in his care.
“They took all my calls and emails — they were happy to set up phone calls to answer questions, and Dr. Pollock was available to me 24/7. These doctors didn’t make me communicate only via MyChart. I had their cellphone numbers. That personal touch and availability was huge. And I felt like I made an informed decision based on knowing a team that was ready to have more power in the surgical room than they might need.”
A life-changing outcome
When Knisely had his surgery in May 2020, it turned out the team did require every one of those talented hands to take care of him — but they were more than prepared.
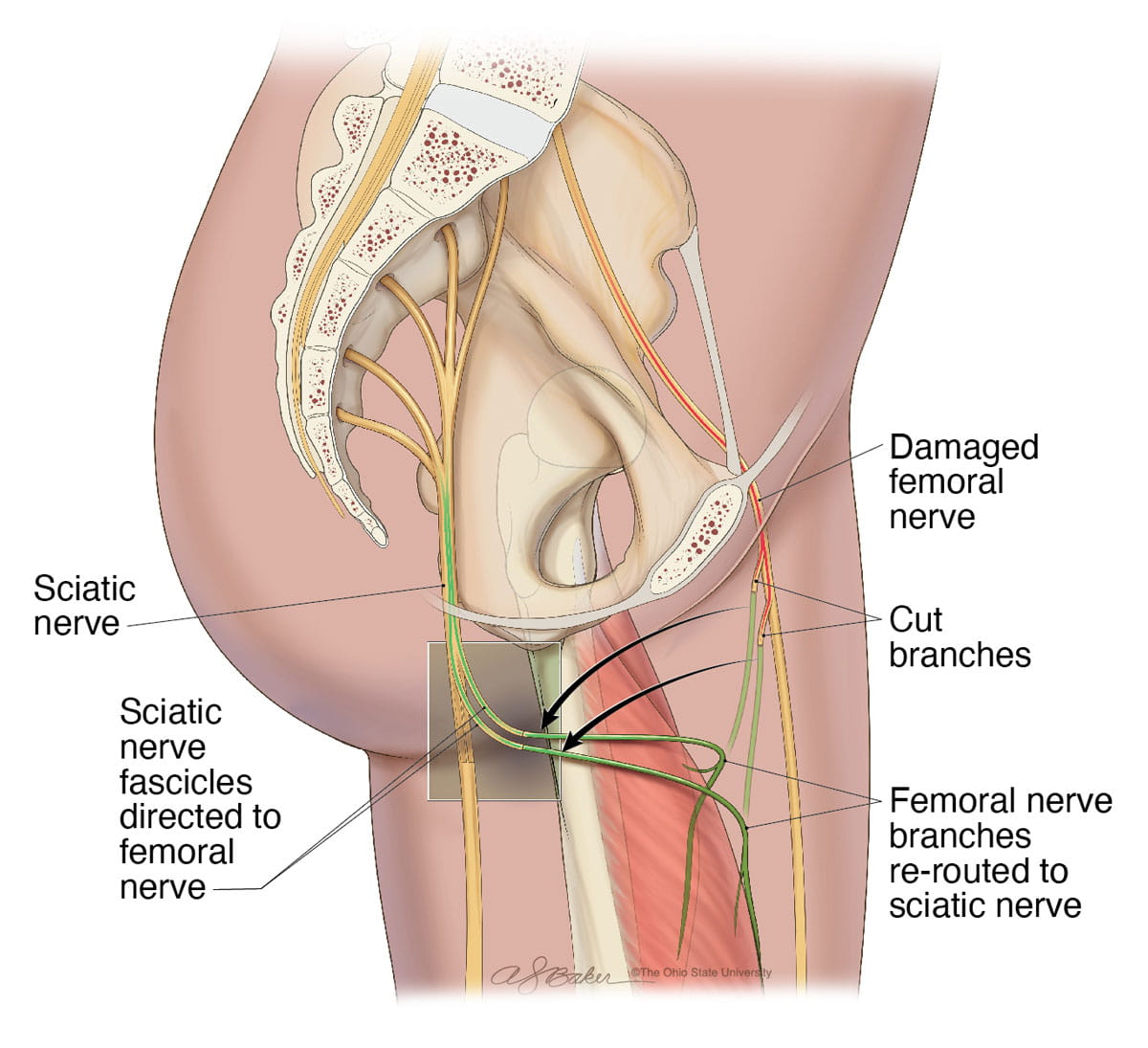
Moore reconstructed the damaged nerve portion that had to be removed and, with her help, Knisely gained back almost complete muscle function of that leg over the next several months.
“Each month, I’ve gotten better, and Dr. Moore says I’ll probably continue to improve for two years post-surgery,” he says.
“I’ve been driving, I can walk up stairs normally. I’m back to 10,000 steps a day. I can chase my grandchildren on the beach.
"I’ve gotten most of my function back, I’m not on any pain medication and I’m able to comfortably sleep through the night. I live a pretty high quality of life."
Knisely is confident that the decision to get this important care from Ohio State will affect his quality of life for the next 20 to 30 years.

“At Ohio State, the patient wins”
When Moore arrived at Ohio State in fall 2019 to begin building her clinical practice, it became clear to her that Ohio State is focused on patient-centered care, she says.
“Our goal is to make their experience a priority, and that comes from the staff who greet them when they check in all the way to post-operative care with our physician assistants and nursing staff,” she says. “The patient is our focus, and that’s why we are so collaborative on a daily basis — it takes a team to provide great care, and our patients deserve that.”
Knisely says he thinks often of what today would look like if he’d gone elsewhere for his care.
“I have no doubt that other places would’ve gotten the tumor out and addressed the underlying threat from cancer, but I don’t know if they would’ve been able to do nerve grafts successfully at a later time. That preparation and having Dr. Moore in the room to do that extensive work has changed my life.”
They both think that’s the key differentiator for Ohio State patients.

“Because we’re so collaborative, the patient wins,” Moore says.
“The patient gets expertise from oncology, reconstructive surgery, pain specialists — I could go on and on. But because of the opportunities to collaborate among all these disciplines, it is at Ohio State that the patient will win.”







