BLVR procedure for COPD, emphysema gives normalcy to patients who once struggled with everyday tasks
Bronchoscopic Lung Volume Reduction (BLVR) dramatically improving life for patients with lung disease
One frigid afternoon in November, April Muldrow, 62, strolled through Blacklick Woods Metro Park in Reynoldsburg, Ohio. Despite the wind chill, she was smiling as she told her story of a lifelong battle with Chronic Obstructive Pulmonary Disease (COPD), which she developed as a result of a genetic disorder.
For years, she struggled to go up and down steps. Carrying groceries or doing anything strenuous was nearly impossible. An oxygen tank was her constant companion. Strolling through a neighborhood park, as she did on this November day, would have been out of the question.
“It was hard for me to breathe; I was basically confined to the house,” Muldrow says.
That was before she met Christian Ghattas, MBBCh, for the first time at The Ohio State University Wexner Medical Center. Dr. Ghattas, a clinical professor of Internal Medicine at The Ohio State University College of Medicine, is her soft-spoken, unassuming interventional pulmonologist who primarily sees patients suffering from severe lung and chest diseases. He’s an expert in helping patients with these diseases live longer, higher-quality lives. For Muldrow, that meant performing a cutting-edge procedure called bronchoscopic lung volume reduction (BLVR).

Dr. Ghattas’ work puts him at the forefront of a pulmonary medical treatment that is giving many patients, including Muldrow, their lives back. After approval from the Food and Drug Administration in 2018, Dr. Ghattas was one of the first doctors in the nation to perform the bronchoscopic lung volume reduction (BLVR) procedure. This minimally invasive surgery opens the tiny airways that become obstructed in patients suffering from COPD symptoms and emphysema and can dramatically improve their lives. Today, the Ohio State Wexner Medical Center is among just a handful of medical centers in the Midwest performing BLVR, and completing more procedures than any other location in Ohio.
The widespread impact of COPD and emphysema
Though Muldrow suffers from a genetic disorder that causes COPD, it is typically an incurable disease resulting from excessive smoke exposure. In the United States, exposure usually comes from smoking cigarettes, and according to the Centers for Disease Control and Prevention, COPD impacts 16 million Americans. Exposure causes inflammation inside the lungs, injury and thickening of airways and the obstruction of smaller airways in the lungs.
“In some patients with COPD, there is destruction of the lung tissue itself, which we call emphysema,” explains Dr. Ghattas. Another three million in the United States have been diagnosed with emphysema, according to the American Lung Association.

Small tasks of daily life become enormous with COPD
Imagine a small, over-inflated balloon that’s tied shut where the air can’t escape. This is what it’s like in the lungs of patients with COPD. Because the lungs aren’t functioning properly to take oxygen into the blood and remove excess carbon dioxide the lungs can become hyperinflated. Hyperinflation pushes the lungs down on the diaphragm muscle beneath the lungs, limiting deep breaths and additionally creating shortness of breath. Not only can the patient not get enough oxygen into the bloodstream from the lungs, it makes it impossible to take deep breaths to increase that oxygen.
Patients with severe COPD and emphysema are often resigned to very sedentary lives, hooked to oxygen tanks for daily survival and feeling a constant state of exhaustion. And though they typically live for many years with medical and oxygen treatments, their quality of life can be extremely poor with options for treatment limited.
There is no cure for patients with these diseases, only medical treatments that can help improve their symptoms. That’s one reason Dr. Ghattas decided to dedicate his life to what he calls a “sub- sub- specialty” of interventional pulmonology medicine.
“Being able to help my patients breathe better is very rewarding and brings joy to my life,” he says.
Dr. Ghattas, who was born, and earned his first medical degree, in Egypt, found his calling before he began his residency training in the United States. He met Thomas Gildea, MD, at the Cleveland Clinic, one of the leading experts in the field and a mentor for Dr. Ghattas still today.
After years of interventional pulmonary fellowships and training — where he also learned to place valves for BLVR procedures — Dr. Ghattas began work at The Ohio State University Wexner Medical Center in 2018. He says it has been a perfect fit and a rare opportunity to perform his specialized work, in large part because the academic health center provides a high volume of patients. On a typical workday, he can see about 20 patients. Several might require BLVR and other procedures offered by interventional pulmonologists.
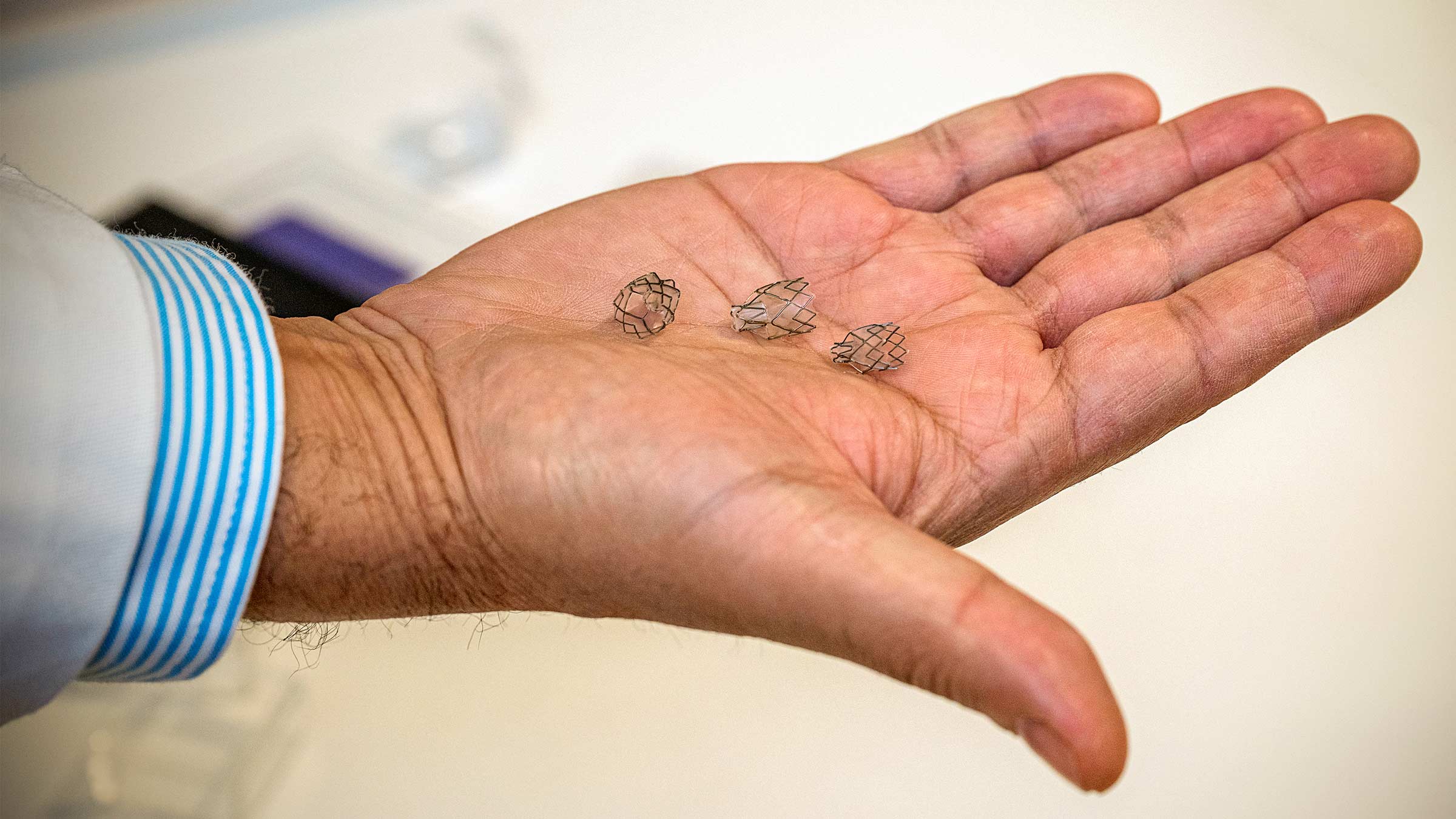
BLVR’s tiny metal cages open airways
BLVR was approved by the FDA in 2018 after nearly 20 years of study. In 2019, Dr. Ghattas began performing his first procedures on patients at Ohio State. In many ways, BLVR is an ideal alternative to more invasive procedures such as lung volume reduction surgery (LVRS), which removes parts of the patient’s damaged or hyperinflated lungs, and a lung transplant, which is a last resort for most others.
BLVR, on the other hand, is performed by placing tiny silicone and metal caged valves in the small airways of a diseased and damaged part of the hyperinflated lung. During the procedure, anywhere from two to seven valves are placed using a scope, or thin tube with a light and camera, to guide the surgeon down the patient’s airway to the target locations. The valves are designed to allow air to flow only one way — out of the overinflated lung.
“Think of the valves we put in the patient’s lungs as a check valve on a car tire,” explains Dr. Ghattas. “When the patient breathes in, the valves close to prevent air from reaching the damaged part of the lung. When the patient exhales, the valves reopen to release trapped air. Over time, that diseased portion of the lung deflates and gets smaller.”
BLVR removes pressure on the diaphragm, improving overall breathing mechanics and lung function, and allows the healthy parts of the lungs to more easily do their job of circulating oxygen into the bloodstream.
Recent studies examining BLVR are incredibly promising. A March 2022 article in the journal Respiratory Medicine found that median survival time for patients undergoing BLVR was 8.6 years — significantly longer than for patients not treated with BLVR (6.8 years) — and that BLVR “was found to be an independent predictor of survival.”
Short term, researchers conducting another study in the Netherlands also saw no negative events six and 12 months after BLVR and experienced “sustained improvements in lung function and quality of life” for at least 24 months.
Results such as these are significant because BLVR is typically performed only on patients in the later stages of COPD and emphysema, when other medical interventions including medications, oxygen tanks and pulmonary rehab are no longer effective at reducing or relieving symptoms.
Bringing BLVR to Ohio State
Muldrow was one of those patients. She was born premature at six months in 1960 on the east side of Columbus and suffered from respiratory issues her entire life. In and out of the hospital as a young girl, she was put on a regimen of respiratory inhalers, medications and allergy shots that never did much good. When she was 35, on a chance visit to an allergist with her daughter, the doctor noticed Muldrow’s severe symptoms and with some additional tests discovered she had Alpha-1 antitrypsin deficiency, an inherited genetic disorder that can cause lung disease and emphysema.
This set Muldrow on a frustrating path of one-step forward, two-steps back for decades.
Her first treatment regimen kept her symptoms at bay until about 2012, when she ultimately needed 4-6 liters of oxygen a day just to get by. That’s when she was referred to Ohio State for a lung transplant, and in 2014, received a new right lung.
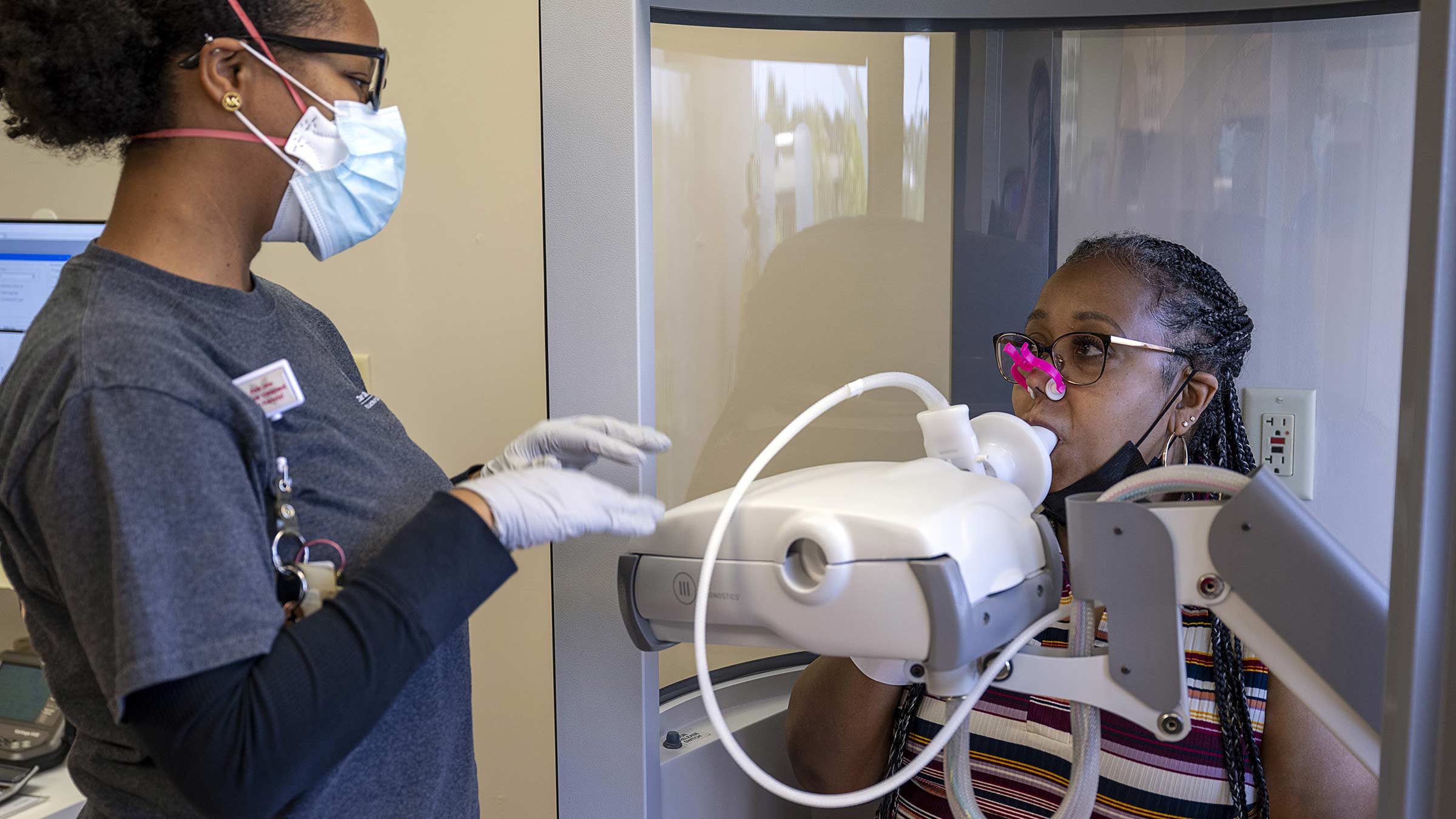
The lung transplant was life-altering. She visited the Columbus Zoo for the first time and could walk the entire park herself. She rode rollercoasters again and started a bucket list of activities and states to visit with her newfound freedom.
Things went very well for another five years, but Muldrow’s left lung became more and more damaged from her genetic condition, forcing the transplanted lung to do most of the work. She began to experience shortness of breath, and ultimately couldn’t perform even basic physical activities, even while on two liters of oxygen per day.
“I’d lived with this my entire life, so I was resigned to feeling this way again,” says Muldrow.
However, a couple of good years had given her a taste of what her life could be like if she could actually breathe freely.
In late 2020, she met Dr. Ghattas, who explained the BLVR procedure and how it might help her, but cautioned a second lung transplant could be a possibility if BLVR wasn’t an option.
“I talk to patients at least three times before this procedure,” says Dr. Ghattas. “And we begin the screening process to ensure that the patient is a good candidate, and prepare them for the procedure.”
“Dr. Ghattas was so informative, gave me the pros and cons of the procedure and was able to answer all of my questions,” says Muldrow. “I was hesitant at first and worried it wouldn’t work, but decided it wouldn’t hurt to try [BLVR],” she says.
Muldrow’s BLVR procedure took place in May 2021, and she became one of the first in the world to have both a lung transplant and BLVR.
Today, she’s able to go to the grocery store and walk her dogs. She washes her car and goes to the local Planet Fitness for her own version of pulmonary rehab at least twice a week.
She’s back to building, and checking off, that bucket list.

“If I’m not exercising, I’m doing tons around the house,” says Muldrow. “I keep myself busy and moving!”
Dr. Ghattas agrees that activity can help patients’ lungs continue to perform, and he’s been impressed with Muldrow’s continued physical activity.
“April was such a unique case with the prior lung transplant and is just doing so well,” he says.
Helping patients live better lives
Today, Dr. Ghattas and the pulmonology team — four interventional pulmonologists, two advanced practitioners and one interventional pulmonology fellow — regularly screen seven to 10 patients each week for the BLVR procedure.
“Obviously, not every patient will qualify for this procedure,” says Dr. Ghattas. But whether or not they are ultimately treated with BLVR, it’s just as important to get so many of these severe patients into the academic health system, ensuring they are enrolled in a yearly lung cancer screening program to catch cancer early, receiving the most advanced treatment and provided multiple medical options for advanced stage COPD and emphysema.
“There’s so much we can do to help these patients live better lives,” says Dr. Ghattas.
For Muldrow, her life got better and her lungs improved just a few days after her BLVR procedure.
“The little girl in me came out,” she says with a grin.

Suffering with COPD or emphysema?
See if Bronchoscopic Lung Volume Reduction (BLVR) may be an option. Call 614-293-4925.