Proton radiation therapy takes aim at a rare cancer
With a cancerous tumor near his heart, a Pennsylvania man traveled to Ohio State for an alternative to standard radiation.
No one expected the spot on the CT scan.
Close to Jim DiCostanzo’s heart, a tumor appeared.
The 5-centimeter mass grew behind DiCostanzo’s sternum, where his thymus gland had been until it gradually shrank and turned into fatty tissue, which happens as people age. Early in life, the thymus is most active, producing white blood cells as part of the immune system.
DiCostanzo had the scan to check if plaque had built up in the arteries to his heart.
“I went into it hoping to avoid taking a statin and came out with a cancer diagnosis,” says DiCostanzo, a native of Pittsburgh.
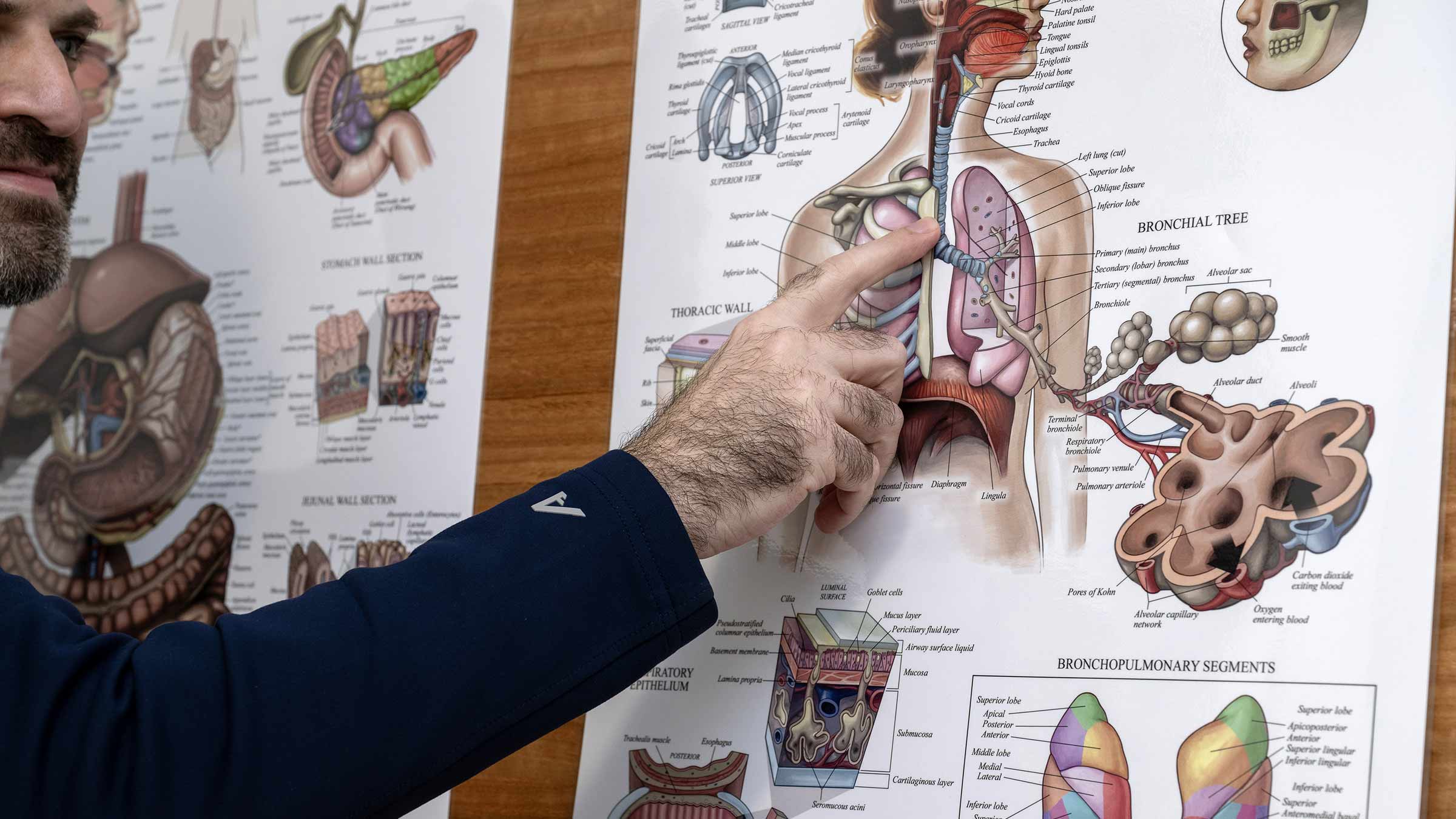
The cancer he never felt coming
Both rare and aggressive, thymic cancer can cause chest pain and trouble swallowing. It can make it hard to breathe. DiCostanzo felt none of that, which isn’t unusual for the cancer early on.
After the surgery to remove the tumor in April 2024, DiCostanzo’s doctor in Pittsburgh recommended radiation.
“I wanted to get radiation as a precaution, since the cancer I had was very aggressive,” DiCostanzo says. “A random cell could have dislodged and traveled to another part of my body.”
Standard radiation, DiCostanzo learned from the radiation oncologist, came with risks for him.
“She said it could affect my lungs, heart and spinal cord, and cause burns on my back.”

When proton radiation is a safer path
Standard radiation might rule out the possibility of cancer returning, but it could also leave him with other problems to vital organs, DiCostanzo worried.
“I didn’t want to destroy the cells in my heart and my lungs and my spine. I was leaning toward just not getting radiation,” DiCostanzo says.
DiCostanzo’s son, Dominic, suggested another option, a different type of radiation: proton radiation therapy. In this highly precise form of cancer treatment, charged particles called protons directly target cancer cells, limiting radiation damage to healthy cells and organs nearby.
Dominic DiCostanzo, PhD, knows the science behind proton radiation better than many. He’s the administrative director of the Proton Therapy Center at The Ohio State University Comprehensive Cancer Center – Arthur G. James Cancer Hospital and Richard J. Solove Research Institute (OSUCCC – James) in Columbus.
The elder DiCostanzo’s local medical center in Pittsburgh didn’t offer proton therapy, nor did any other hospitals in the area, he says. From Pittsburgh, the closest proton radiation centers in Pennsylvania are in Lancaster or Philadelphia.

Besides being closer, the OSUCCC – James not only has the technology for proton radiation but also has highly skilled staff members with expertise in using this innovative equipment, Jim DiCostanzo would learn.
“It made the decision to move forward with radiation easier for me.”
So, DiCostanzo and his wife, Sandy, drove to the OSUCCC – James and met with Jeremy Brownstein, MD, a radiation oncologist.
Before the tumor was removed, it had grown into the fiber sac over DiCostanzo’s heart.
“The fact that the cancer had invaded that barrier indicates that there might have been other cancer cells we didn’t know about, so radiation was necessary,” Dr. Brownstein says.
Proton radiation would be best, he told DiCostanzo, to keep his heart from getting much, if any, radiation.
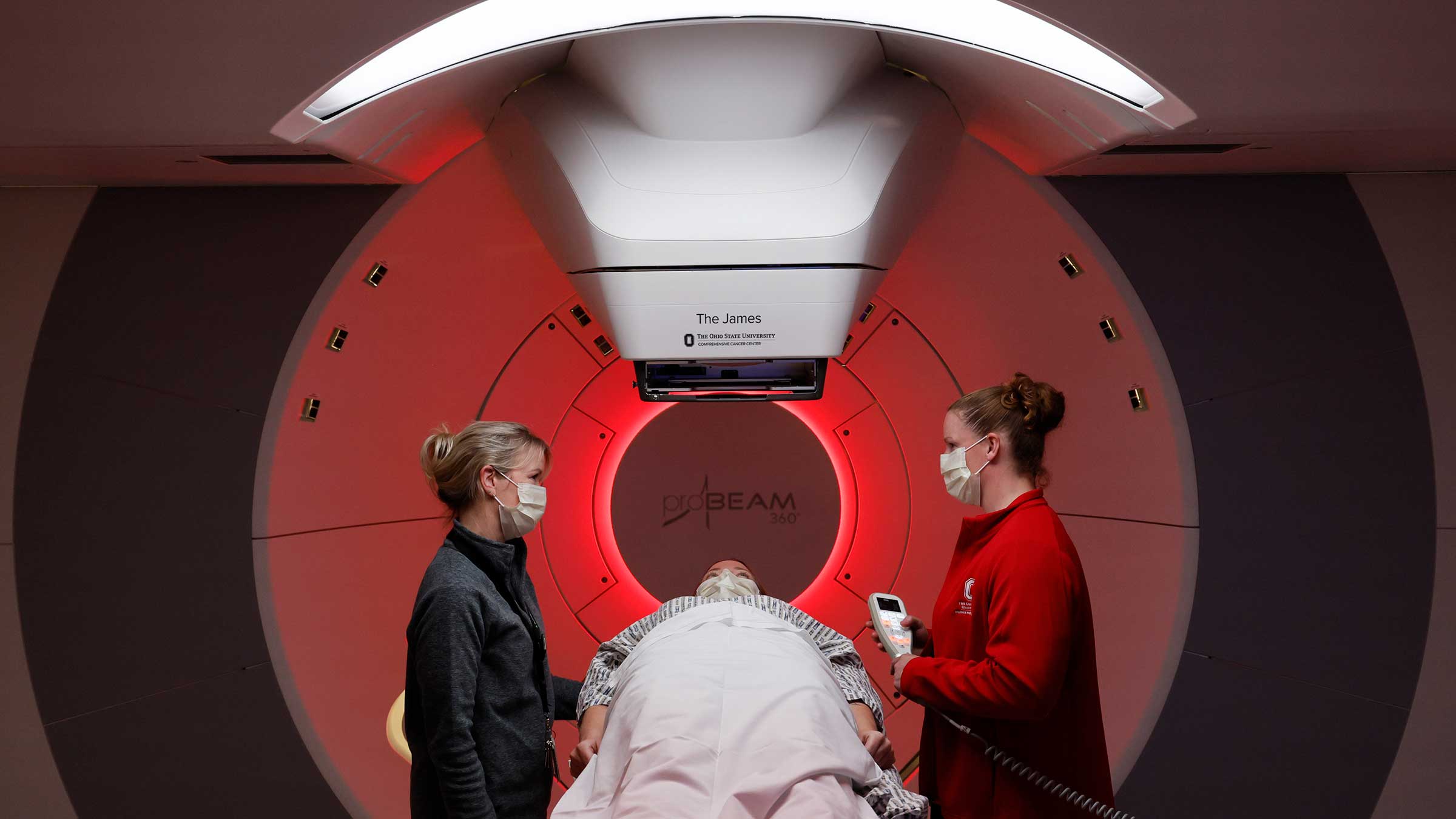
How proton radiation therapy works
Radiation kills cancer cells by damaging their DNA, the buildings blocks for cells. It can cut in half the risk of cancer returning, Dr. Brownstein says.
What’s different about proton radiation therapy compared to standard radiation is that it uses protons – charged particles that are parts of atoms – while standard radiation uses X-rays.
With proton radiation, the protons travel only a certain distance into the body before they stop. They deliver the highest dose of radiation at the end of their path, the tumor.
“It’s like rolling a hot coal on a piece of wood,” Dr. Brownstein says. “As it slows down, it burns the wood more and more, and where it stops, it burns a hole in it. What we’re trying to do is to make all of those protons stop at the tumor and deposit most of their dose there.”
Experts calculate how far the protons need to go into the body to reach the target. They go a little beyond their target to reduce the odds of potentially missing it.
With standard radiation, X-rays pass through the body, reach the tumor and continue through the body, exiting the other side. The dose of X-rays decreases as the beams move through the body.
“It works phenomenally,” Dr. Brownstein says of standard radiation. “But there is excess dose going to normal cells nearby because each of these beams is still going clear through the patient.”
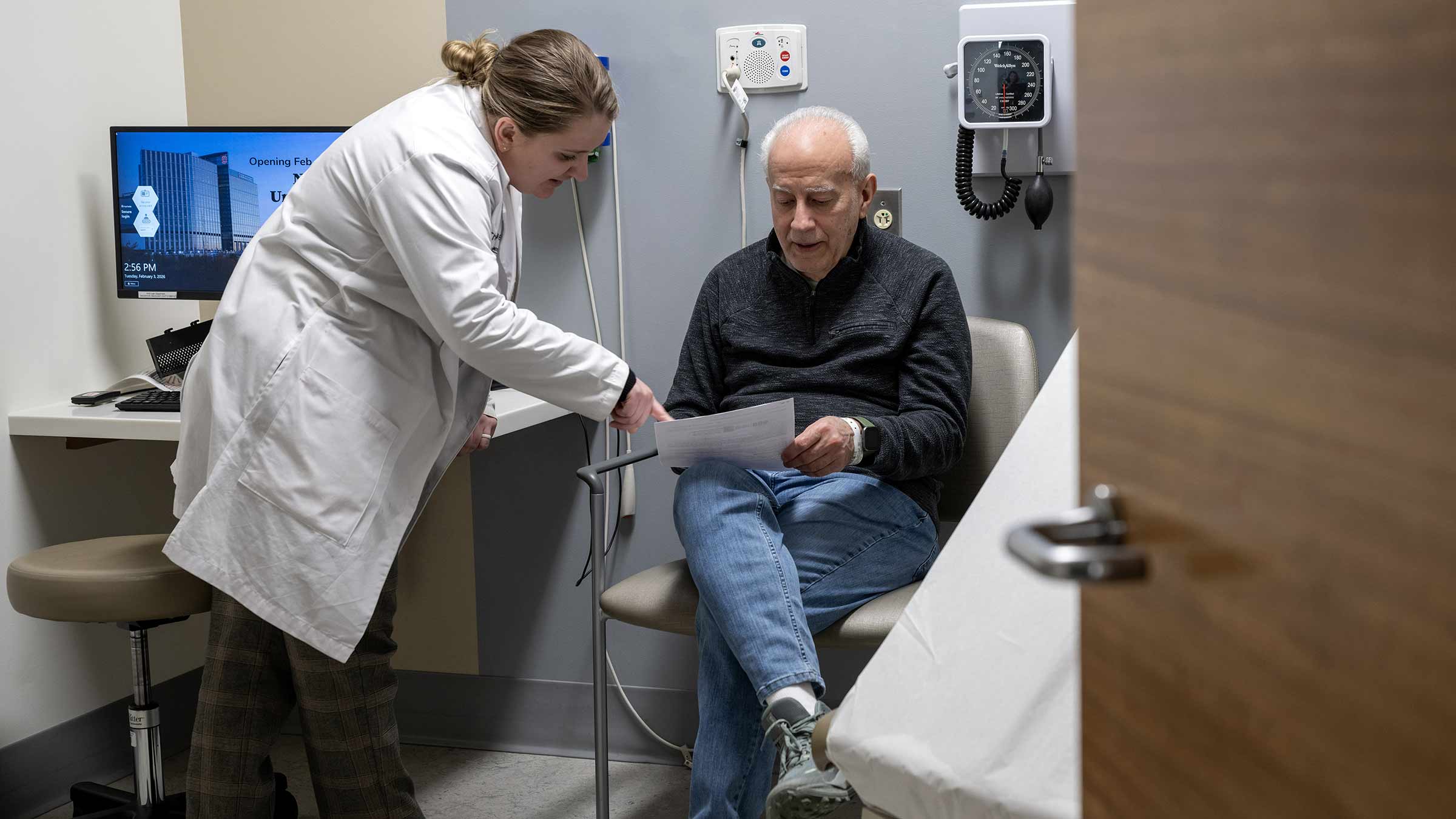
Proton radiation vs. standard radiation
Doctors often use proton therapy on children with brain or spine cancers to avoid exposing nearby developing organs to radiation. In adults, proton therapy is commonly used for targeting cancer anywhere in the head, neck or spine. It’s also a frequent option when cancer returns after earlier radiation treatment.
If someone is going to receive very high doses of radiation but few treatments, standard radiation likely would be a better choice. That’s because proton radiation is delivered based on experts’ estimates of how deep the area is where the tumor cells may be. If the proton particles don’t reach the site of the targeted area during each of those few sessions, the radiation may not kill off all the cancer cells.

‘No evidence the cancer is still around’
In the summer of 2024, Jim and Sandy rented a home in Columbus while he had 25 days of proton radiation therapy. They took long daily walks at parks for the first few weeks before afternoon naps replaced those walks. Radiation left him tired, but that was only temporary, and DiCostanzo considers it a small price to pay for being cancer-free.
“Potentially, it was lifesaving for me,” says DiCostanzo, 76, a retired marketing analyst for PNC Financial.

Every three months, DiCostanzo returns to the OSUCCC – James for another scan to know if cancer has come back. He has always left relieved.
“Best we can tell, there’s no evidence the cancer is still around,” Dr. Brownstein says. “We don’t say ‘cured’ until a decade goes by without cancer returning.”
However, the longer DiCostanzo goes without the cancer, the better his chances are that it won’t return, Dr. Brownstein says.
An aggressive cancer doesn’t take long to grow. So, if there were any leftover cancer cells after the radiation treatments, it’s more likely the aggressive cells will form a tumor early on rather than several years later.
That offers DiCostanzo enough reassurance he no longer thinks about cancer much. Many friends prayed for him through the process, and every now and then, they ask how he’s doing.
“And then I think, ‘Oh yeah, I had cancer.’ It’s not top of mind for me anymore.”





